Diagnosis of OCD (Obsessive Compulsive Disorder)
Getting an accurate OCD diagnosis is the first step toward effective treatment and relief from intrusive thoughts and repetitive behaviours. A proper evaluation helps distinguish OCD from anxiety or other conditions and guides the right therapy or medication plan.

Option #1. Start with a Psychiatrist
Recommended if you are unsure whether you have OCD, OCD along with another condition, a different mental health concern, or no diagnosable condition at all
Process:
- Choose a Psychiatrist of your preference and schedule an initial evaluation session.
- During this session, the Psychiatrist will conduct a detailed clinical assessment to understand your symptoms, history, and overall mental health.
- Based on this evaluation, the Psychiatrist may:
- Provide a diagnosis for OCD and begin a discussion around treatment and management options, or
- Recommend follow-up sessions for further evaluation, or
- Refer you to a Clinical Psychologist for specialised OCD assessments and diagnostic tools, if required.
Any additional sessions or referrals are aimed at arriving at the most accurate and well-rounded diagnosis.
Outcome:
By the end of this process, you will either:
- Receive a confirmed diagnosis of OCD (with clarity on next steps for treatment), or
- Learn that you do not meet the diagnostic criteria for OCD, with professional insight into what else may be contributing to your experiences.

Option#1. Consult a Psychiatrist
-
Psychiatrist
Prerna Maheshwari
Specializing in diagnosing and managing addiction, depression, anxiety, ADHD, autism, OCD
Prerna Maheshwari -
Psychiatrist
Dr. Pankhuri Monga
Gold-medalist psychiatrist & sexual health expert for anxiety, mood, relationships, wellbeing.
Dr. Pankhuri Monga -
Psychiatrist
Dr Milan Nathvani
Compassionate psychiatrist with expertise in CBT for depression, OCD, and substance use disorders
Dr Milan Nathvani -
Dr Miller

Option #2. Start with a Clinical Psychologist
Recommended if you suspect you may have OCD
Process:
- Book an OCD Diagnosis Package with a Clinical Psychologist of your choice.
- The Clinical Psychologist will conduct 1–3 sessions, which may include detailed clinical interviews and gold-standard psychological assessments, depending on their approach.
- Based on this evaluation, the Clinical Psychologist will determine whether the criteria for an OCD diagnosis are met.
- A comprehensive assessment report will be shared and discussed with you.
- The cost of the OCD Diagnosis Package covers the entire assessment process, from evaluation to report discussion.
Outcome:
At the end of the process, you will either:
- Receive a confirmed diagnosis of OCD, or
- Gain clarity that you do not meet the criteria for OCD, along with professional insight into what may be contributing to your concerns.

Common Questions around Diagnosis
-

What is OCD?
Therapist Response -

Who can diagnose OCD?
Therapist Response -

What are the common early signs and when to consider a diagnosis?
Therapist Response -

What is the step-by-step process of seeking an OCD diagnosis?
Therapist Response -

What to expect during an assessment for OCD?
Therapist Response -

What are the challenges and barriers in getting diagnosed for OCD?
Therapist Response -

Why does an OCD diagnosis matter?
Therapist Response -

What happens after diagnosis of OCD? Give me treatment options and next steps.
Therapist Response -

How to deal with co-morbid conditions and misdiagnosis of OCD?
Therapist Response -

How to differentiate OCD from other mental health conditions?
Therapist Response
What is OCD?
Therapist Response:
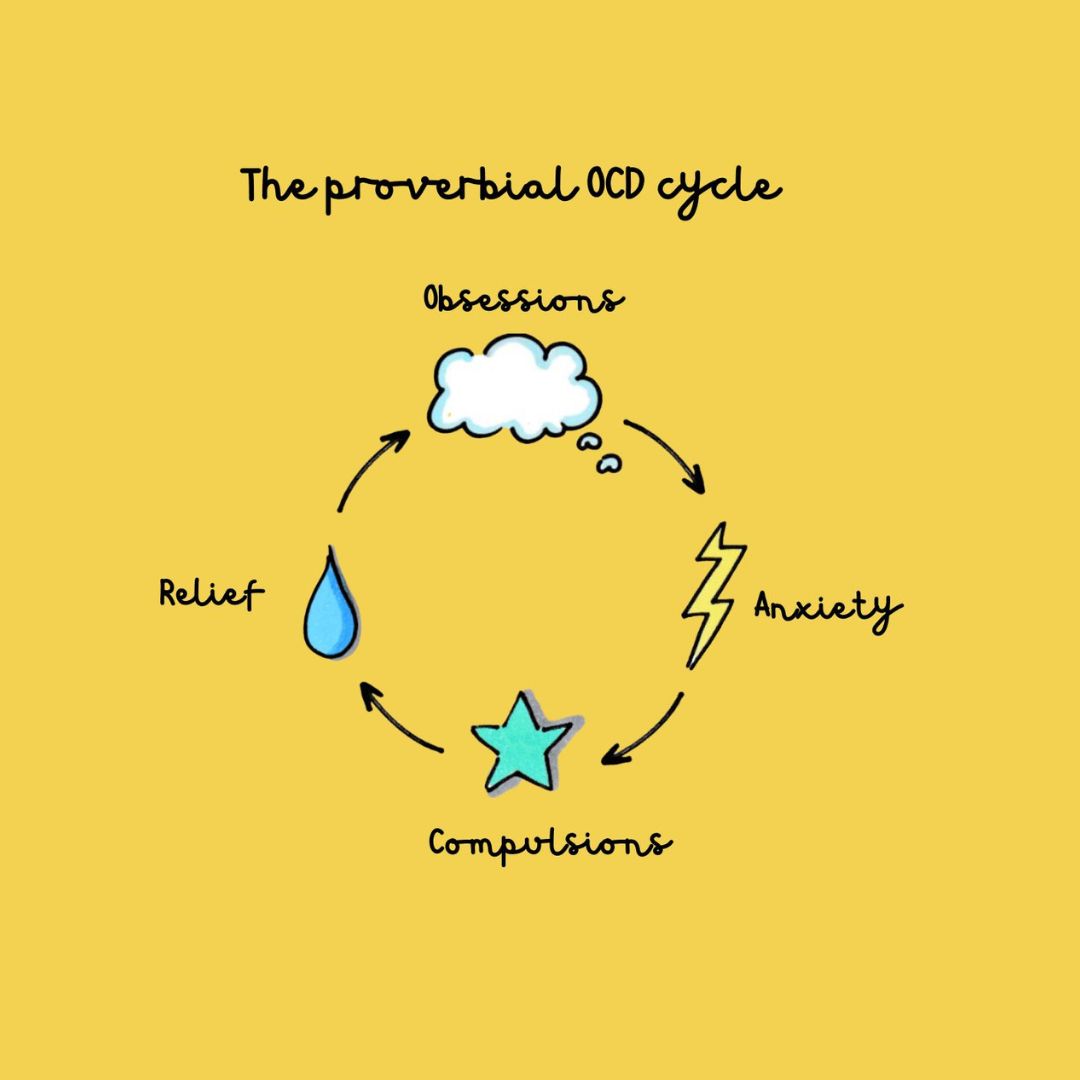
Obsessive-Compulsive Disorder (OCD) is a mental health condition where a person experiences persistent, unwanted thoughts or urges (obsessions) and/or engages in repetitive behaviours or mental acts (compulsions) to relieve the distress caused by those thoughts. What makes it different from occasional worry or habit-forming is that the thoughts/behaviours are time-consuming, cause significant distress and interfere with your daily life.
Obsessions
Obsessions are repeated, intrusive thoughts, images, or fears that keep coming back and are hard to control. They’re not the same as normal worries as they feel sticky, irrational, and anxiety-provoking.
For example: A person may keep thinking “What if I left the door unlocked and someone breaks in?” even after checking several times. Another might feel “If I don’t wash my hands again, I could make someone sick.” Some people may fear that thinking a “bad” thought during prayer could bring harm to their loved ones.
Even when they realise these thoughts are unrealistic, it’s very hard to stop them.
Compulsions
Compulsions are the actions or rituals done to reduce the anxiety caused by obsessions. They bring temporary relief, but the thoughts soon return and restart the cycle.
Some examples are: Repeatedly checking if the gas knob or main door is locked; washing hands again and again, even when they’re already clean; repeating a prayer or counting in a certain way to “cancel out” a bad thought.
These acts don’t actually prevent harm but in the moment, they make the person feel safer or calmer.
In short: OCD = Obsessions (distressing thoughts) + Compulsions (repetitive behaviours to feel better)
Who can diagnose OCD?
Therapist Response:
Both psychiatrists and clinical psychologists can formally diagnose OCD - they just look at it from different angles.
Psychiatrists (medical doctors in mental health) use diagnostic criteria (according to ICD/DSM) to assess symptoms, look at OCD through a biological and neurological lens, rule out medical or substance-related causes, and can prescribe medications such as SSRIs if needed.
Clinical psychologists (with a professional license from RCI) also use the same diagnostic criteria (ICD/DSM) but rely more on psychometric assessments, detailed interviews, standardized tests, and behavioral observations to understand the psychological patterns behind obsessions and compulsions. They map out the symptom profile, severity and any comorbid issues.
Post diagnosis, when it comes to facilitating therapy - that’s typically the domain of counselling psychologists or therapists. They employ modalities like CBT or ERP. While they help with screening and psychoeducation, they cannot prescribe any medicines or provide a formal diagnosis. However, many clinical psychologists in India are also trained and licensed to provide psychotherapy, particularly when they specialize in behavioural or trauma-focused work. So, while diagnosis may be their formal responsibility, many clinical psychologists also continue the treatment process themselves, bridging both assessment and therapy.
So, in India, either a psychiatrist or clinical psychologist can be your first point of contact for diagnosis, depending on access. While psychiatrists are often easier to reach, both are appropriate and commonly collaborate.
What are the common early signs and when to consider a diagnosis?
Therapist Response:
OCD often starts small - maybe with thoughts or habits that seem ordinary at first. You may find yourself rechecking the gas knob, rearranging things until they feel “just right,” or worrying about contamination after touching a doorbell. But gradually, these thoughts and behaviours begin to take over more time and mental space. Thus, the key thing to notice is how much distress or interference they cause in your everyday life.
Early signs may include intense doubt, guilt, or fear of causing harm, feeling compelled to repeat tasks until they feel perfect, or avoiding certain situations altogether - like refusing to cook out of fear of making someone ill. You might be aware that the thoughts are unreasonable, but still feel powerless to stop - and that’s a telling sign!
So, it’s worth considering a diagnosis when these thoughts and rituals take up significant time, cause distress, or interfere with work, studies, relationships, or rest. If you find that your day is dictated by your need to check, clean, count, or mentally “fix” something just to feel okay, it may be time to reach out to a mental health professional for assessment.

What is the step-by-step process of seeking an OCD diagnosis?
Therapist Response:
Start by noting what you or your family observe: the intrusive thoughts, the rituals, how long they take, and how much they disrupt your life. Then, book an appointment with a qualified mental-health professional (a psychiatrist or an RCI-registered clinical psychologist).
On your first visit to a psychiatrist, they will evaluate your symptoms, decide whether the pattern of obsessions and compulsions meets diagnostic criteria, and prescribe medication if needed. If medical causes are suspected, a psychiatrist may order basic tests or refer you to a physician.
In case you first go to a clinical psychologist, they will carry out detailed assessments (through interviews, questionnaires, behavioural observation) to understand how your thoughts, feelings and rituals are functioning. Using a clinical interview, the clinician will ask about your symptoms, medical history, mood, sleep, substance use, and family history. This way, they help clarify and confirm whether it’s OCD or something similar, and often work with the psychiatrist to co-create the treatment plan. After assessment, the clinician will confirm whether your symptoms meet diagnostic criteria and discuss treatment options (therapy like CBT/ERP, medication if needed, or both).
Following this, you’re directed to a therapist or counselling psychologist who then supports you through structured therapy, especially evidence-based approaches like Cognitive Behavioural Therapy (CBT) and Exposure and Response Prevention (ERP). They help you face your fears, reduce your rituals, build coping strategies and gradually improve daily functioning.

What to expect during an assessment for OCD?
Therapist Response:
An OCD assessment is more like a detailed conversation than a medical test. The professional (a psychiatrist or clinical psychologist) will first ask you to describe what’s been bothering you: the kinds of thoughts that keep repeating, the actions or rituals you feel compelled to do, and how they affect your daily life. You might be asked when the symptoms started, how intense they are, and what triggers or relieves them.
Along with this conversation, the clinician may use standard questionnaires or rating scales to measure the severity of your symptoms. They may also explore related concerns like anxiety, mood changes, or sleep issues, since these often occur alongside OCD.
The aim isn’t to judge, but to understand your experience in depth so that the professional can confirm whether it fits the pattern of OCD and plan the right treatment. Most Indian clinics now blend structured tools with warm, open dialogue to make the process comfortable and collaborative.

What are the challenges and barriers in getting diagnosed for OCD?
Therapist Response:
Getting an OCD diagnosis in India can be difficult for many reasons. One major challenge is lack of awareness. People often mistake OCD for a personality trait, like being “too clean” or “a perfectionist,” rather than a mental health condition. Because of this, many delay seeking help until symptoms start severely affecting their work or relationships.
Even religious or cultural practices in India, such as ritual purity or repeated prayers, can mask OCD symptoms.
Stigma and fear of judgment can also hold people back. Discussing intrusive thoughts - especially if they involve taboo themes like religion, sex, or harm - can feel shameful or “wrong.” Many might worry that sharing these thoughts will make others question their character or sanity.
Access is another common barrier. Clinical psychologists and psychiatrists are concentrated in urban areas, leaving smaller towns and rural regions with limited options. The cost of private consultations, language barriers, and long waiting periods in government hospitals can further add to the difficulty.
Finally, family misunderstanding can play a significant role too. Relatives may think that the person “just needs to relax” or “pray more,” rather than recognising OCD as a legitimate, treatable condition.

Why does an OCD diagnosis matter?
Therapist Response:
Getting a formal OCD diagnosis can feel like a relief, because it gives a name to what you’re experiencing. It helps you understand that your intrusive thoughts and compulsive behaviors are not personal flaws, but part of a recognized condition that many people live with.
A diagnosis also opens the door to effective treatment, including therapy (like CBT or ERP) and, when needed, medication prescribed by a psychiatrist.
Beyond treatment, a diagnosis provides legitimacy and clarity, which can help family, friends, or workplaces understand your struggles better. For example, loved ones may be more patient if they realize that certain rituals aren’t choices but compulsions, and schools or employers can make reasonable accommodations. In India, where mental health awareness is still growing, having a formal assessment can also reduce self-blame and make it easier to seek support confidently, rather than suffering in silence.

What happens after diagnosis of OCD? Give me treatment options and next steps.
Therapist Response:
Once you have a formal OCD diagnosis, the next step is planning treatment, tailored to your symptoms and daily life. Usually, a psychiatrist and clinical psychologist collaborate to decide the best approach. For many, the first line of treatment is Cognitive Behavioural Therapy (CBT), specifically Exposure and Response Prevention (ERP), where you gradually face your fears while learning to resist compulsions. This helps retrain your brain’s response to obsessive thoughts.
If your symptoms are severe or significantly disrupt daily life, a psychiatrist may prescribe medication, commonly SSRIs (selective serotonin reuptake inhibitors), which help reduce the intensity of obsessions and compulsions. Therapy and medication often work best together.
After starting treatment, you’ll have regular follow-ups to track progress, adjust strategies, and address any emerging challenges. Family involvement and understanding can also be crucial, especially in India, where living arrangements often involve multiple family members. With consistent support, most people see meaningful improvement.
Beyond individual therapy and medication, support groups and therapy groups can also play a vital role in recovery after an OCD diagnosis. Living with OCD often brings feelings of shame, exhaustion, or loneliness, and these emotions can be eased when you meet others who truly understand what it’s like. Being part of a space where people openly discuss their struggles, coping strategies, and small victories can offer reassurance and hope. It helps normalize the experience and reminds individuals that they are not defined by their disorder. OCD support groups allow members to share lived experiences, discuss specific subtypes (like contamination or checking OCD), explore fears around heredity, or simply find acceptance among those who “get it.” These conversations can complement formal therapy by providing ongoing emotional support and practical coping insights.
Lastly, adherence to treatment (whether medication, therapy, or lifestyle changes) is key. Recovery from OCD is gradual, and consistency matters far more than speed. Staying connected to both professionals and peers can help you stay motivated through setbacks and celebrate progress along the way.

How to deal with co-morbid conditions and misdiagnosis of OCD?
Therapist Response:
OCD often doesn’t appear alone - it frequently coexists with other mental health conditions like anxiety, depression, ADHD, or even certain personality disorders. Because of overlapping symptoms, misdiagnosis can happen, especially if only one set of symptoms is noticed. For instance, someone might be labelled as “just anxious” when it is the underlying OCD that is driving the worry and rituals.
So, the key is to seek a thorough assessment from a qualified professional, i.e., a clinical psychologist or psychiatrist, who can evaluate for both OCD and any other conditions. Additionally, keeping a detailed symptom diary (noting intrusive thoughts, compulsions, triggers, mood changes, sleep, and daily functioning) can help professionals get an accurate picture.
In India, where access to mental health specialists can be uneven, it may help to ask for a second opinion or approach multidisciplinary clinics (e.g., NIMHANS) where psychiatrists and psychologists collaborate. This is because early and accurate identification of comorbidities ensures a treatment plan that addresses all aspects of your mental health, rather than focusing on only one symptom.

How to differentiate OCD from other mental health conditions?
Therapist Response:
OCD can often be mistaken for other disorders because many of them involve anxiety, repetitive behaviours, or rigid thinking. But what makes OCD stand out is the involuntary, distressing nature of its thoughts and the strong urge to neutralize them through rituals or actions. People with OCD usually recognize that their fears and thoughts are irrational but still can’t stop themselves from acting on them, which brings intense guilt or exhaustion.
For instance, in Generalized Anxiety Disorder (GAD), worries are more broad-based - about work, relationships, or the future, whereas OCD thoughts are highly specific and intrusive, like “If I don’t chew my food thirty times, something terrible will happen.”
In perfectionism or Obsessive-Compulsive Personality Disorder (OCPD), individuals genuinely value order and control. These traits feel natural and ego-syntonic (aligned with one’s sense of self). In OCD, however, the compulsions feel unwanted and burdensome, something the person wishes they could stop.
OCD may also resemble body-focused disorders like Body Dysmorphic Disorder (BDD) or health anxiety, but again, the compulsions in OCD (like mirror checking or reassurance seeking) stem from intrusive, unwanted fears rather than vanity or general worry.
Looking for OCD Support? Here are some options to consider.
1-on-1 Therapy for OCD
Work with a therapist to challenge intrusive thoughts, manage compulsions, and develop healthier thinking patterns around OCD.
Therapist-Led Support Groups for OCD
Join one of our therapist-led groups to connect with others working through OCD challenges and learn coping strategies.
Peer Conversations on OCD
Select from verified peers who’ve lived with OCD to feel understood and exchange practical ways to cope.
Workshops
Explore expressive arts, journaling, or drama therapy workshops to channel anxiety and regain a sense of control over your OCD.

Unsure of your next steps?
Book an Exploratory Call with one of our therapists to gain initial insights, practical solutions, and personalized guidance on the best options for your needs.

Related Self-Assessments
-
Self-Assessment for Panic Disorder
Take the TestIdentify signs of panic attacks and evaluate how frequently and intensely they occur, to know if further professional evaluation is needed.
-
Test for Anxiety
Take the TestMeasure your anxiety levels accurately using the GAD scale—a trusted assessment tool providing insights into your current emotional state
-
Overthinking
Take the TestDiscover if overthinking might be impacting your life with our quiz designed to gauge your thought patterns and tendencies.














